DEFINITION
Atrioventricular (AV) dissociation occurs when two completely independent pacemaker sites become active and compete with one another. In most cases, the sinus node provides one pacemaker, while an ectopic focus—usually ventricular—provides the other. Less commonly, two ectopic pacemakers may compete.
Although most dissociation involves pacemakers in different chambers (atria and ventricles), it is also possible—though rare—for both pacemaker foci to arise within the same chamber (e.g., sinus node vs. an atrial ectopic focus, or two independent junctional pacemakers).
The faster pacemaker will dominate, but the relative rates often allow impulses from both pacemakers to intermittently activate the ventricles.
In the accompanying article, AV dissociation occurs during a ventricular tachycardia (VT), which helps secure the diagnosis.
Can You Really Recognize AV Dissociation During a Ventricular Tachycardia?
Jerry W. Jones, MD FACEP FAAEM
CEO and Chief Instructor | Medicus of Houston
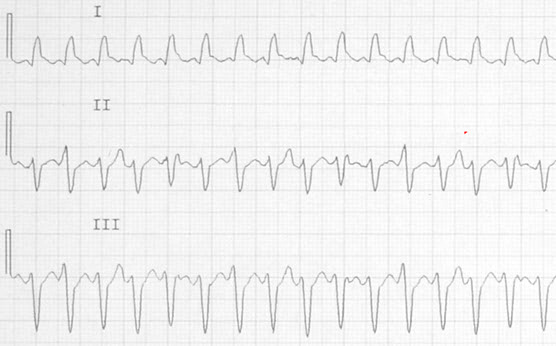
Recognizing AV Dissociation Within the Tachycardia
Most clinicians have only a vague idea of what they are looking for when scanning a wide complex tachycardia for signs of AV dissociation. This is not a simple task. It requires study, training, and a clear mental roadmap. AV dissociation will not be obvious, and it certainly will not jump out at you. You must look for it — and you must know exactly what you are looking for.
AV dissociation occurs when the atrial rhythm—usually sinus—continues to depolarize independently while a ventricular ectopic rhythm competes for control. Occasionally, a sinus impulse manages to conduct through the AV node and His bundle, reaching the ventricles when they are sufficiently repolarized. When this happens, the atrial impulse produces a conducted QRS complex: a capture beat.
What does a capture beat look like?
You will see:
- An upright P wave (in all leads except aVR, where it is normally inverted)
- Followed by a QRS complex
- The QRS is usually narrower than the ectopic ventricular beats
- The PR interval may be normal or slightly prolonged
- The key feature: the QRS appears early and out of sync with the ventricular tachycardia.
Capture beats are always early — never late.
Many online examples incorrectly label late beats as “capture beats.” Those are simply sinus beats occurring after the VT pauses. True capture beats interrupt the VT rhythm.
AV Dissociation vs. VA Dissociation
AV dissociation has a cousin: VA dissociation.
VA dissociation may or may not indicate VT.
AV dissociation, however, almost always indicates VT.
It is often taught as “absolute proof” of VT. It is not absolute — but the supraventricular rhythms capable of producing true AV dissociation are so rare that most clinicians will retire without ever seeing one. For practical purposes, AV dissociation is considered diagnostic of VT.
So What Are We Looking For?
1. Disturbances in the Ventricular Rhythm
Look for a QRS that appears slightly too early.
A preceding P wave may or may not be visible; it is often buried in the T wave of the previous beat.
2. QRS Morphology: Onset, Termination, and T Wave
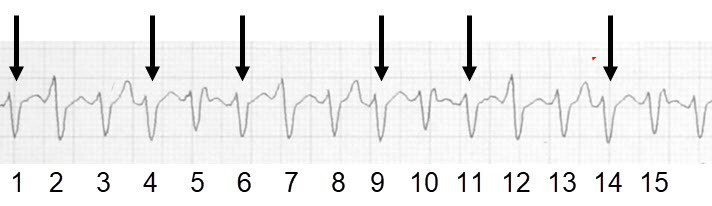
In the Lead II rhythm strip the arrowed QRS complexes represent the ventricular ectopic rhythm.
- Compare QRS #2 with QRS #4.
QRS #2 has a tall, wide initial r wave — not just an r wave, but an r wave plus a sinus P wave superimposed. - Look at the T wave after QRS #3.
It is larger than the T wave after QRS #4 because it contains a T wave plus a sinus P wave. - Compare the termination (J‑point) of QRS #5 with QRS #4.
Again, the difference is due to a superimposed sinus P wave.
These are the exact places where sinus activity hides during AV dissociation.
3. Know What the P Waves Should Look Like
Sinus P waves should be upright in all leads except aVR.
If a QRS appears early, it is likely a capture beat — even if the P wave is not visible.
During rapid rhythms, P waves are frequently swallowed by T waves. Always inspect the T wave of the preceding beat.
If you see a clear P wave followed by a QRS at a conductible PR interval — but the QRS appears late — that is not a capture beat. The VT simply paused long enough for normal conduction to occur. VT is notoriously paroxysmal.
4. Fusion Beats — The Most Subtle Indicator
Fusion beats are sinus‑conducted beats that activate the ventricles simultaneously with the ventricular ectopic focus. Because only part of the ventricles are captured, the resulting QRS is a hybrid.
Fusion beats:
- May look almost identical to the VT QRS complexes
- Are often slightly narrower
- Can be extremely subtle
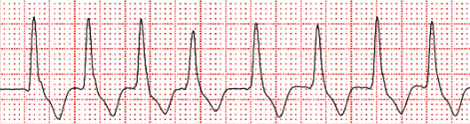
The fusion beat is the 4th beat — a small but real deviation from the surrounding VT morphology.
